Understanding the Hormonal Shift: Premenopause to Perimenopause
Understanding the Hormonal Shift: From Premenopause to Perimenopause
Millions of women navigate the menopausal transition every year, yet many are caught off guard by how early it can start, how wide-ranging the symptoms can be, and just how much their hormones are doing behind the scenes. This post is made to help you break down the key hormones involved, how they change during perimenopause, and what you can expect to feel along the way.
First, the Foundation: What a "Normal" Cycle Looks Like
Before we talk about perimenopause and menopause, it helps to understand the baseline of what hormones do in a typical premenopausal cycle.
In a regular premenopausal 28-day cycle, four hormones choreograph a precise monthly sequence — estradiol (E2), progesterone, follicle-stimulating hormone (FSH), and luteinizing hormone (LH). Each one has a distinct role and a predictable rhythm.
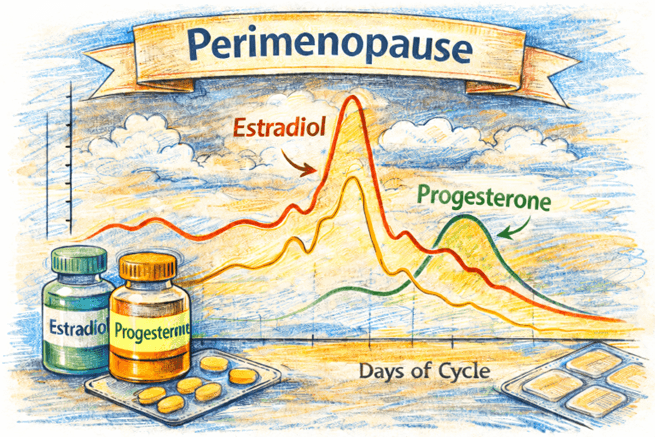
Estradiol (E2) is the primary form of estrogen in reproductive-age women. It rises steadily through the first half of the cycle (the follicular phase), peaking just before ovulation, then drops and rises again more gently during the luteal phase before falling sharply at menstruation. Estradiol does far more than manage reproduction — it affects mood, bone density, cardiovascular health, skin elasticity, sleep quality, and cognitive function.
Progesterone is very low to non-existant in the first half of the cycle, then surges dramatically after ovulation. It is produced by the corpus luteum (the remnant of the follicle that released the egg). Its job is to prepare the uterine lining for potential implantation of an egg and to support early pregnancy. If no pregnancy occurs, progesterone drops sharply, triggering menstruation. Progesterone also has a calming, sleep-promoting effect on the brain.
FSH (Follicle-Stimulating Hormone) is released by the pituitary gland to stimulate the ovaries to develop follicles (each containing an egg). It rises early in each cycle to "recruit" follicles, then quiets once a dominant follicle takes over. Think of FSH as the pituitary's way of sending a message to the ovaries to “get things started.”
LH (Luteinizing Hormone) builds steadily through the follicular phase, then surges dramatically around Day 13–14. This surge happens after the estradiol peak around day 12. This LH surge is the direct trigger for ovulation — without it, the egg is never released. After ovulation, LH quickly falls back to baseline.
This four-hormone system works in harmony when ovarian reserve is healthy and the ovaries respond predictably. However, as the amount of eggs decline with age, so does this synchronicity of hormones.
What Is Perimenopause — and When Does It Start?
Perimenopause is the transitional period leading up to menopause. It can begin anywhere from the late-30s to the early 50s, with most women entering it in their mid 40s. The average duration is 4 years although this varies from woman to woman.
By definition, perimenopause is a gradual decline in ovarian reserve — the number and quality of remaining eggs. Women are born with roughly 1 million follicles; by puberty that's dropped to around 300,000–500,000, and by the mid-40s the supply is running low. As the follicles diminish in number and quality, the ovaries become less responsive — and the entire hormonal cascade begins to fall apart.
The Hormonal Changes of Perimenopause
FSH: The First Signal
The earliest measurable hormonal change in perimenopause is a rise in FSH. This happens because the ovaries, with fewer high-quality follicles remaining, also produce less inhibin B — a hormone that normally signals the pituitary to slow down FSH production. Without that feedback, the pituitary increases FSH output, essentially "shouting louder" to try to stimulate the ovaries.
Elevated FSH (generally above 10–15 mIU/mL on Day 3 of a cycle, though labs vary) is one of the earliest clinical markers of the transition. As the transition advances, FSH continues to rise as the pituitary works overtime trying to make the ovaries respond and release an egg (although fewer and fewer are present).
Estradiol: The Unpredictable Hormone
Contrary to what most people think, estradiol doesn't simply decline steadily during perimenopause. Instead, it becomes wildly erratic. In early perimenopause, estradiol levels can actually be higher than in a typical premenopausal cycle, as the elevated FSH over-stimulates whatever follicles remain, sometimes triggering exaggerated surges. This is then followed by steep drops — creating dramatic swings that can happen within days.
This volatility is responsible for many of the most disruptive perimenopausal symptoms. It's not just low estrogen that causes problems — it's the rapid changes in estrogen level that the body struggles to adapt to.
As perimenopause progresses toward menopause, the overall trend is downward, with increasingly low and flat estradiol levels and fewer and fewer ovulations.
Progesterone: The Underappreciated Hormone
Progesterone is the first hormone to meaningfully decline in perimenopause. Because progesterone is only produced in significant amounts after ovulation, any cycle that is anovulatory (where no egg is released) results in essentially no progesterone rise that month.
In perimenopause, anovulatory cycles become increasingly common — the follicle may develop and even produce estradiol, but then fail to release an egg. The result: the uterine lining is exposed to estrogen without the balancing effect of progesterone. This can lead to a misbalance between estrogen and progesterone which leads to heavier and more irregular periods because of the relative excess of estrogen.
Beyond reproduction, progesterone loss affects sleep, anxiety levels, and mood regulation.
LH: The Blunted Surge
The LH surge that is critical for triggering ovulation, becomes increasingly unreliable during perimenopause. Even when it occurs, it may be smaller in magnitude and less precisely timed. In fully anovulatory cycles, the classic midcycle LH spike is absent altogether.
What You Might Feel: Symptoms by Hormone
Understanding which hormone is shifting can help make sense of seemingly unrelated symptoms.
Symptoms Driven by Estradiol Fluctuation
Hot flashes and night sweats
Vaginal dryness and discomfort
Brain fog and memory lapses
Mood swings
Headaches and migraines
Joint pain
Skin and hair changes
Symptoms Driven by Progesterone Loss
Sleep disturbances
Anxiety and irritability
Heavier, longer, or more irregular periods
Spotting between periods
What to Expect With Your Period
Very early in perimenopause, even if cycles remain mostly regular, mild reductions in progesterone can occur that can lead to sleep and mood issues. As the transition into perimenopause progresses, women begin to notice changes in their cycle. Most commonly periods shorten. Later, cycles begin to lengthen and become unpredictable, sometimes skipping months entirely. Flow can be heavier in some cycles (because of the relatively higher estrogen compared to progesterone) and lighter or absent in others (anovulatory cycles).
The hallmark of approaching menopause is missed periods — first occasional, then more frequent, until they stop entirely. Menopause is when you have not had a period for 12 months.
A Note on Individual Variation
It's worth emphasizing that the perimenopausal experience is strongly individual. Some women sail through with minor symptoms; others find the transition profoundly disruptive to quality of life. The timing, intensity, and pattern of symptoms depend on genetics, body composition, lifestyle factors (stress, sleep, exercise, diet), and whether any underlying conditions are present.
Hormone levels during perimenopause are also highly variable from day to day — a single blood test can be misleading. Symptoms and cycle history are often more informative than a snapshot lab result.
Understanding these hormonal fluctuations, and knowing just how early they can occur, can help you navigate the symptoms you're having. No one person is created the same. What you're experiences is uniquely your own — and deserving of care, attention, and answers.

Written by
Katie Hart
My blog



